
The hip joint (HJ) is a complex joint formed by several bones: the femur, pubis, ilium, and ischium.It is surrounded by the periarticular bursa and a powerful muscle-ligamentous corset, protected by subcutaneous fat and skin.
The ilium, ischium, and pubis form the pelvic bone and are connected by hyaline cartilage at the acetabulum.These bones fuse together before the age of 16.
A distinctive feature of the femoral joint is the structure of the acetabulum, which is covered with cartilage only in the upper part and partially on the side.The middle and lower segments are occupied by adipose tissue and the femoral ligament, enclosed in a synovial membrane.
Reason
Pain in the hip joint can be caused by damage to intra-articular elements or nearby structures:
- skin and subcutaneous tissue;
- muscles and ligaments;
- synovial bursa;
- acetabular lip (cartilaginous rim running along the edge of the acetabulum);
- The articular surfaces of the femur or pelvis.
Pain in the joint area is caused by inflammation or violation of the integrity of its constituent structures.Often, pain occurs when infection enters the joint cavity (infectious arthritis) and autoimmune damage (rheumatoid and reactive arthritis).
Mechanical injuries are also no less common, resulting in damage to the epiphyses of bones, ligaments, synovial membranes and other tissues.Active people and athletes who experience high physical activity are more susceptible to injury.
Also at risk are elderly people who have pain in the pelvic bones due to degenerative-dystrophic changes in the cartilage, as well as children and adolescents during periods of hormonal changes.
Pain in the hip joint on the left or right side is caused by metabolic diseases – for example, diabetes mellitus, pseudogout and obesity.
The full list of possible diseases is as follows:
- Perthes disease;
- Arthrosis;
- Koenig's disease;
- diabetic arthropathy;
- Pseudogout;
- intermittent hydroarthrosis (intermittent ascites of the joints);
- chondromatosis;
- Reactive, rheumatoid and infectious arthritis;
- Juvenile epiphysiolysis;
- Injuries.
perthes disease
With Perthes disease, the blood supply to the femoral head is disrupted, leading to aseptic necrosis (death) of the cartilage tissue.Most often children under 14 years of age, mostly boys, are affected.
The main symptom of Perthes disease is persistent pain in the hip joint, which increases with walking.Children often complain that their leg hurts from the hip and they start limping.
In the early stages, symptoms are mild, leading to late diagnosis, when impression (intra-articular) fracture has already occurred.The destructive process is accompanied by increased pain, swelling of soft tissues, and stiffness in limb movement.The patient cannot rotate, rotate, bend, or straighten the hip externally.It is also difficult to move the leg to the side.
Disturbances in the autonomic nervous system are also observed: the feet become cold and pale with excessive sweating.Sometimes the body temperature rises to low fever levels.
Note: In Perthes disease, the lesion may be unilateral or bilateral.In most cases, one of the joints hurts less and heals faster.
arthrosis
Osteoarthritis of the hip joint is called coxarthrosis and is diagnosed mainly in elderly people.The disease progresses slowly, but causes irreversible changes.The pathological process begins with damage to the cartilage, which becomes thinner as a result of the increased thickness and viscosity of the synovial fluid.
The development of coxarthrosis leads to joint deformity, muscle atrophy and significant limitation of movements up to complete immobility.Pain syndrome with arthrosis has a wave-like (non-constant) nature and is localized on the outer side of the thigh, but can spread to the groin, buttocks and lower back.
In the second stage of arthrosis, painful sensations cover the inner side of the thigh and sometimes extend to the knee.As the disease progresses, the pain in the hip becomes more intense and sometimes subsides only with rest.
Coxarthrosis can be primary and secondary.Primary coxarthrosis develops against the background of osteochondrosis or arthrosis of the knee.Preconditions for secondary coxarthrosis may be hip dysplasia, congenital hip dislocation, Perthes disease, arthritis and traumatic injuries (dislocations and fractures).
koenig's disease
If the thigh hurts on the side of the joint, the cause may be death of cartilage tissue (necrosis) - Koenig's disease.The disease most often affects young men aged 16–30, who complain of pain, decreased range of motion, and periodic "jamming" of the foot.
Koenig's disease develops in several stages: first, the cartilage tissue softens, then hardens and begins to separate from the articular surface of the bone.In the third or fourth stage, the necrotic area is rejected and enters the articular cavity.This causes accumulation of effusion (fluid), stiffness in movement, and blockage in the left or right joint.
Reference: The presence of a "joint mouse" in the hip joint leads to the development of coxarthrosis.
diabetic arthropathy
Osteoarthropathy, or Charcot joint, is seen in diabetes mellitus and is characterized by progressive deformity with pain of varying intensity.Painful sensations are weakly expressed or completely absent, since with this disease sensitivity sharply decreases due to pathological changes in nerve fibers.
Diabetic arthropathy occurs during long-term diabetes and is one of its complications.This often occurs in women who did not receive full treatment or it was ineffective.It is worth noting that the hip joints are extremely rarely affected.
pseudogout
As a result of calcium metabolism disorders, calcium crystals begin to accumulate in the joint tissues, and chondrocalcinosis, or pseudogout, develops.The disease got its name due to the similarity of symptoms to gout, which is characterized by its paroxysmal course.
Acute and sharp pain appears suddenly: the affected area becomes red and swollen, and becomes hot to the touch.The attack of inflammation lasts from several hours to several weeks, then everything goes away.With chondrocalcinosis, pain on the left or right side of the pelvis is possible.
In the vast majority of cases, pseudogout occurs for no apparent reason, and it is not possible to detect calcium metabolism disorders even during examination.Presumably, the cause of the disease is a local metabolic disorder inside the joint.In one patient out of a hundred, chondrocalcinosis develops against the background of existing systemic diseases – diabetes, renal failure, hemochromatosis, hypothyroidism, etc.
synovial chondromatosis
Chondromatosis of the joints, or cartilaginous island metaplasia of the synovium, primarily affects the large joints, including the hip.Most often, this pathology occurs in middle-aged and elderly men, but there are also cases of congenital chondromatosis.
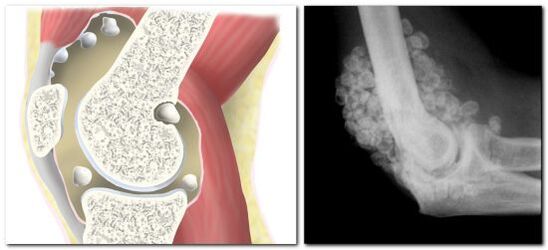
With chondromatosis, the synovial membrane transforms into cartilage or bone tissue, resulting in the formation of chondromic or bone bodies up to 5 cm in size in the joint cavity.
The clinical picture of insular metaplasia is similar to arthritis: the patient is bothered by pain in the hip bone, mobility of the leg is limited, and a characteristic crunching sound is heard when walking.
Since chondromatosis is a dysplastic process with the formation of chondromic bodies, the phenomenon of “articular mouse” cannot be ruled out.In this case, the "mouse" can get stuck between the articular surfaces of the bones, causing partial or complete blockage of the joint.The joint remains blocked until the chondromic body enters the lumen of the capsule, and only then is motion fully restored.
Help: Frequent or prolonged jamming of joints can provoke the development of coxarthrosis.Complications of synovial chondromatosis are stiffness (shrinkage) and muscle atrophy.
Arthritis
Arthritis is an inflammation that is localized in the articular surfaces of the acetabulum and femur.Damage to the hip joint is called cochitis, which causes mild pain in the back of the thigh and groin area.
There are several types of arthritis, the most common type affecting the hip joint is the infectious form.Other types are diagnosed much less frequently.What causes infectious arthritis?Pathology begins to develop after bacteria and viruses enter the joint cavity.
The clinical picture of infectious arthritis may vary depending on the type of microorganism causing it.However, there are 5 characteristic symptoms that are seen in all patients:
- Pain in the joint of the right or left leg (bilateral damage can also occur);
- swelling and inflammation at the joint;
- redness of the skin;
- decreased motor ability;
- Increase in body temperature.
At the beginning of the disease, patients experience severe pain, especially when standing from a sitting position.The joint hurts almost constantly;The pain makes it impossible to stand or sit.It should be noted that the infectious form of arthritis is always accompanied by fever, chills, headache, weakness and nausea.
juvenile epiphysiolysis
The term epiphysiolysis literally means decay, destruction of the articular surface of the bone, or more precisely, of the cartilage covering it.A characteristic feature of such damage is the cessation of bone growth in length, which leads to asymmetry of the lower extremities.
In adults, epiphysiolysis occurs when there is a fracture with displacement or rupture of the epiphysis.Destruction of the epiphyses in the growth zone is possible only in adolescence, which is why the disease is called juvenile.
Juvenile epiphysiolysis is an endocrine-orthopedic pathology based on an imbalance between growth hormones and sex hormones.It is these two groups of hormones that are essential for the normal functioning of cartilage tissue.
The predominance of growth hormone over sex hormone leads to a decrease in the mechanical strength of the growth zone of the femur bone, and displacement of the epiphysis.The last part of the bone is located below and behind the acetabulum.
Typical symptoms of epiphysiolysis include pain on the right or left side of the thigh (depending on which joint is affected), lameness, and unnatural position of the leg.The leg pain radiates outward, the muscles of the buttocks, thighs and legs become atrophied.
treatment
For the treatment of Perthes disease, chondroprotectors are prescribed to promote cartilage regeneration and angioprotectors are necessary to improve blood circulation.Complex therapy also includes massage, exercise therapy, physiotherapy - UHF, electrophoresis with calcium and phosphorus, mud and ozokerite applications.
Patients with Perthes disease are advised to unload the limb and use orthopedic devices (plaster casts), as well as special beds to prevent deformity of the femoral head.
What to do and what medicines to take for arthrosis depends on the stage of the disease.The following measures help relieve pain and slow down the disease process in stages 1-2:
- Non-steroidal anti-inflammatory drugs (NSAIDs);
- Vasodilators;
- Muscle relaxants to relax muscles;
- Chondroprotectors;
- hormonal (for severe pain);
- Ointments and compresses with anti-inflammatory or chondroprotective effects.
Patients at stage 3-4 are advised to undergo surgery.
Koenig's disease can only be treated surgically;During arthroscopic surgery the affected part of the cartilage is removed.
Treatment of diabetic arthropathy includes correction of the underlying disease – diabetes mellitus, wearing special unloading bandages and taking medications.All patients, regardless of the stage of the disease, are prescribed antiresorptive drugs – bisphosphonates, as well as products containing vitamin D and calcium.To relieve pain and inflammation, drugs of the NSAID group and corticosteroids are prescribed.If there are infectious complications, a course of antibacterial therapy is carried out.
There is no specific treatment for pseudogout;During exacerbations, anti-inflammatory drugs are prescribed.A large amount of fluid accumulated in the joint is an indication for intra-articular puncture, during which the fluid is drained and corticosteroid medications are given.
Chondromatosis of the hip joint requires mandatory surgical intervention, the amount of which depends on the scale of the lesion.If the number of chondromic bodies is low, they are removed by partial synovectomy (excision of the synovial membrane) or minimally invasive arthroscopy (through three punctures).Surgical treatment of the progressive form of chondromatosis can only be radical and is performed using open arthrotomy or complete (total) synovectomy.
Therapy for acute infectious arthritis includes applying a plaster to the hip joint area, taking drugs of various groups (NSAIDs, antibiotics, steroids).When a purulent process develops, a course of medical punctures is performed to cleanse the joint.
Treatment of juvenile epiphysiolysis is surgical only.During the operation, closed repositioning of the bones is performed using skeletal traction.The jointed parts of the bones are then joined with pins and grafts.
Absolutely all pathologies of the hip joint are serious diseases that require mandatory medical supervision.Any injury that occurs with severe pain, limited mobility, and changes in joint configuration after a fall or trauma requires emergency medical attention.If there is no traumatic injury, but pain of varying intensity in the joint occurs regularly, you need to make an appointment with a therapist or rheumatologist and be examined.


























































































